23.2 Health History Basic Concepts
Open Resources for Nursing (Open RN)
During a health history, the nurse collects subjective data from the patient, their caregivers, and/or family members using focused and open-ended questions. Before discussing the components of a health history, let’s review some important concepts related to assessment and communicating effectively with patients.
Subjective Versus Objective Data
Obtaining a patient’s health history is a component of the Assessment phase of the nursing process. Information obtained while performing a health history is called subjective data. Subjective data is information obtained from the patient and/or family members and can provide important cues about functioning and unmet needs requiring assistance. Subjective data is considered a symptom because it is something the patient reports. When documenting subjective data in a progress note, it should be included in quotation marks and start with verbiage such as, “The patient reports…” or “The patient’s wife states…” An example of subjective data is when the patient reports, “I feel dizzy.”
A patient is considered the primary source of subjective data. Secondary sources of data include information from the patient’s chart, family members, or other health care team members. Patients are often accompanied by their care partners. Care partners are family and friends who are involved in helping to care for the patient. For example, parents are care partners for children; spouses are often care partners for each other, and adult children are often care partners for their aging parents. When obtaining a health history, care partners may contribute important information related to the health and needs of the patient. If data is gathered from someone other than the patient, the nurse should document where the information is obtained.
Objective data is information observed through your senses of hearing, sight, smell, and touch while assessing the patient. Objective data is obtained during the physical examination component of the assessment process. Examples of objective data are vital signs, physical examination findings, and laboratory results. An example of objective data is recording a blood pressure reading of 140/86. Subjective data and objective data are often recorded together during an assessment. For example, the symptom the patient reports, “I feel itchy all over,” is documented in association with the sign of an observed raised red rash located on the upper back and chest.
Addressing Barriers and Adapting Communication
It is vital to establish rapport with a patient before asking questions about sensitive topics to obtain accurate data regarding the mental, emotional, and spiritual aspects of a patient’s condition. When interviewing a patient, also consider the patient’s developmental status and level of understanding. Ask one question at a time and allow adequate time for the patient to respond. If the patient does not provide an answer even with additional time, try rephrasing the question in a different way for improved understanding.
If any barriers to communication exist, adapt your communication to that patient’s specific needs.
For more information, visit the “Communication” chapter in Open RN Nursing Fundamentals.
Cultural Safety
It is important to conduct a health history in a culturally safe manner. Cultural safety refers to the creation of safe spaces for patients to interact with health professionals without judgment or discrimination. Focus on factors related to a person’s cultural background that may influence their health status. It is helpful to use an open-ended question to allow the patient to share what they believe to be important. For example, ask “I am interested in your cultural background as it relates to your health. Can you share with me what is important to know about your cultural background as part of your health care?”
If a patient’s primary language is not English, it is important to obtain a medical translator, as needed, prior to initiating the health history. The patient’s family member or care partner should not interpret for the patient. The patient may not want their care partner to be aware of their health problems or their care partner may not be familiar with correct medical terminology that can result in miscommunication.
A localized pathogen that spreads to a secondary location.
To promote safety for clients of all ages, nurses should be knowledgeable about safety risks according to age and developmental stages because the types and frequencies of accidents vary among age groups. Information from the Centers for Disease Control (CDC) regarding safety tips for each age group is summarized in the following subsections.[1]
Infants and Preschoolers
Drowning is the leading cause of death in children aged 1-3 years. Motor vehicle accidents, falls, choking, and accidental poisoning are also safety concerns for this age group. Infants and toddlers are curious, but they lack the judgement to recognize the dangers of their actions, so childproofing the home and providing adult supervision are essential for this developmental age group.[2] See Figure 5.7[3] for an image of an infant car seat used to protect infants in the event of a motor vehicle accident. Nurses help educate parents about the proper use, positioning, and installation of car seats.

School-Aged Children
In children aged 4-11, motor vehicle injuries are a major cause of unintentional injury, along with drowning and poisoning. This age group is more aware of dangers and limitations, but adult supervision is still important. The nurse should educate parents of school-aged children about safety seats, booster seats, or shoulder seat belts while riding in the car.[4]
Bicycle accidents are also a common concern in this age group. Many bike accidents involve the head or face because of the lack of helmet use. Nurses provide health teaching to school-aged children regarding bicycle safety and helmet use. See Figure 5.8[5] for an image of a girl wearing a bike helmet.

Because this age group is beginning to enjoy more independence, basic instructions and education on how to recognize and respond to potentially dangerous situations with strangers should also be provided. Parents should also be educated about the AMBER alert system that can be activated if a child is missing and believed to be kidnapped or in danger. This AMBER alert system uses the resources of law enforcement and the media to notify the public about a possible abduction or a missing child in danger.[6]
Nurses must also be aware of signs of maltreatment and child abuse because millions of children are affected each year. Child abuse includes physical, sexual, emotional abuse, and neglect. According to the American Academy of Child and Adolescent Psychiatry (AACAP), after abuse or violence, many children develop mental health problems, including depression and post-traumatic stress disorder. These children may also have serious medical problems, learning problems, and problems getting along with friends and family members. Every state has laws that require health care professionals to report suspected child abuse no matter what form this abuse takes.[7]
Adolescents
Motor vehicle accidents are the number one cause of death for adolescents. Teens aged 16-19 are three times more likely to be in a fatal crash than drivers older than age 20. Adolescent males are twice as likely to die in a motor vehicle accident than females of the same age. Texting while driving is a common cause of distracted driving and accidents in adolescents. Because much of an adolescent’s time is spent away from the home, it is difficult for parents to control many of the decisions that adolescents make. Nurses educate teenagers to use seat belts, obey speed limits, and never use a cell phone or text while driving.[8] See Figure 5.9[9] for an image reminding teenage drivers to not text and drive.

Traumatic brain injuries (TBI) may occur in this age group due to participation in sports and recreation-related activities. TBI results from a blow, jolt, or hit to the head that causes a disruption in blood function or flow to the brain. Nurses should always be alert for indications of a concussion when a sports injury has occurred. Signs of a concussion requiring immediate medical attention include the following:
- Headache, vomiting, balance problems, fatigue, or drowsiness
- A dazed and confused appearance or difficulty concentrating or remembering; confusion
- Emotional irritability, nervousness, or a change in personality
The CDC has comprehensive information and education materials for parents, coaches, players, and health care providers as part of their “Heads Up” program.[10]
Substance abuse is another significant concern in the adolescent population and includes substances such as tobacco, alcohol, illicit drugs, prescription medication, over-the-counter medications, and bath salts. The National Institutes of Health provides many resources for educating teens and their parents about substance abuse.[11]
Adults
Intimate partner violence and substance abuse are common safety issues in the adult population.
Intimate Partner Violence
Intimate partner violence (IPV) is widespread in the United States and is the most prevalent adult safety issue. Intimate partner violence includes physical or sexual violence, stalking, and psychological or coercive aggression by current or former intimate partners. Victims can be female or male, and sexual orientation can be heterosexual or LGBTQ+. The nurse is often the initial health care professional in contact with a victim of IPV. Prompt recognition of a potential or actual threat to client and staff safety is crucial. It is often the nurse’s assessment that plays an important role in identifying a client experiencing IPV. Compassion and understanding are important to show to this vulnerable population. Effective communication is necessary to help victims come forward and share their experiences of abuse. IPV is a complex issue, and the client may not initially consider leaving the abuser as an option. See Figure 5.10[12] for an image of a sign in a community demonstrating support against domestic violence.

See the following tools and resources to share with clients experiencing IPV. For example, the Danger Assessment Tool is a self-administered survey that is free to use and is available in several languages.[13] Nurses can refer clients experiencing IPV to the National Center on Domestic Violence, the Trauma and Mental Health database for resources,[14] and the National Domestic Violence Hotline for free, confidential support.[15] Most importantly, nurses should assist clients experiencing IPV to create a safety plan.
View the tools and resources available at these hyperlinks to share with individuals experiencing intimate partner violence:
Substance Abuse
Substance abuse is defined by the World Health Organization (WHO) as a maladaptive pattern of using alcohol and/or drugs despite it causing persistent social, occupational, psychological, or physical problems that can be physically hazardous. Substance abuse continues to be a safety issue that affects adults across all socioeconomic levels. In America over 450,000 people died between 1999 and 2018 as a result of an opioid overdose.[16] The abuse of prescription pain medication (such as oxycontin and fentanyl) and heroin is a national crisis that plagues social and economic welfare. Substance abuse not only affects an individual, but also causes harm to their family members. Early identification of substance abuse, rehabilitation interventions, and continued support are key for helping the individual, as well as their family members, in the recovery process. See Figure 5.11[17] for an image of a heroin needle found in a community setting.

Older Adults
According to the Centers for Disease Control and Prevention, falls and motor vehicle accidents are leading causes of injury in older adults. However, several other issues pose significant hazards for this population, such as fires, accidental overdosing on medications (due to poor eyesight and confusion), elder abuse, and financial exploitation.[18] In most reported cases of elder abuse, a caregiver or a person in trusted relationship is the perpetrator. For various reasons such as fear and disappointment, most of these cases go unreported. Abuse, including neglect and exploitation, is experienced by about 1 in 10 people aged 60 and older who live at home. From 2002 to 2016, more than 643,000 older adults were treated in the emergency department for nonfatal assaults and over 19,000 homicides occurred.[19] Read an example of an older adult experiencing financial exploitation in the following box.
Consider the story of John, a 92-year-old male who lost his wife over a year ago and has been lonely ever since. He lives alone in a large home in the country. John hired a repairman to fix his roof. The repairman befriended John, bringing him homemade cookies and pies and even running errands for him. The repairman often stayed for coffee, and the two of them spent time talking about fishing and gardening. The repairman convinced John to take out a reverse mortgage to pay for additional improvements on his home. Then, knowing John’s bank account numbers and login information, the repairman stole $250,000 that John received for his reverse mortgage.
Most victims of elder abuse are frequently seen in the emergency department several times before they are admitted to the hospital. Nurses must be alert to any indications of elder abuse, such as suspicious injuries or behaviors, and report suspected incidents to local adult protective services agencies. Commons signs of elder abuse or maltreatment include the following[20]:
- Bruises, cuts, burns, or broken bones that are unexplainable or suspiciously explained
- Malnourishment or weight loss
- Poor hygiene, an unkempt appearance, unclean clothing, or dirty, matted hair
- Foul odor from clothing or body
- Anxiety, depression, or confusion
- Unexplained transactions or loss of money
- Withdrawal from family members or friends
View additional resources related to elder abuse in the following box.
Additional resources for older adults suspected as being victims of elder abuse:
An infection that becomes disseminated throughout the body.
The presence of bacteria in blood.
An exaggerated inflammatory response to a noxious stressor (including, but not limited to, infection and acute inflammation) that affects the entire body.
An infection that becomes disseminated throughout the body.
Interpreting Sensations
Before learning about sensory function, it is important to understand how the nervous system works. An intact nervous system is necessary for information to be delivered from the environment to the brain to trigger responses from the body. For neurons to transmit these messages, they are in the form of an action potential. Sensory receptors perceive a stimulus and then change the sensation to an electrical signal so that it can be transmitted to the brain and then out to the body. For example, a pain receptor perceives pain as your hand touches a hot tray. The signal is transmitted to the brain where it is interpreted, and then signals are quickly sent to the hand to pull away from the hot stimuli.[22]
Our bodies interpret sensations through a process using reception, perception, and reaction. Reception is the first part of the sensory process when a nerve cell or sensory receptor is stimulated by a sensation. Sensory receptors are activated by mechanical, chemical, or temperature stimuli. In addition to our five senses, we also have somatosensation. Somatosensation refers to sensory receptors that respond to stimuli such as pain, pressure, temperature, and vibration. It also includes vestibular sensation, a sense of spatial orientation and balance, and proprioception, the sense of the position of our bones, joints, and muscles. Although these sensory systems are all very different, they share a common purpose. They change a stimulus into an electrical signal that is transmitted in the nervous system.[23]
The sensory receptors for each of our senses work differently from one another. Light receptors, sound receptors, and touch receptors are each activated by different stimuli with specialized receptor specificity. For example, touch receptors are sensitive to pressure but do not have sensitivity to sound or light. Nerve impulses from sensory receptors travel along pathways to the spinal cord or directly to the brain. Some stimuli are also combined in the brain, such as our sense of smell that can affect our sense of taste.[24]
As an individual becomes aware of a stimulus and it is transmitted to the brain, perception occurs. Perception is the interpretation of a sensation. All sensory signals, except olfactory system input, are transmitted to the thalamus and to the appropriate region of the cortex of the brain. The thalamus, which is in the forebrain, acts as a relay station for sensory and motor signals. When a sensory signal leaves the thalamus, it is sent to the specific area of the cortex that processes that sense.[25] However, conditions that affect a person’s consciousness also affect the ability to perceive and interpret stimuli.
Reaction is the response that individuals have to a perception of a received stimulus. The brain determines what sensations are significant because it is impossible to react to all stimuli that are constantly received from our environment. A healthy brain maintains a balance between sensory stimuli received and those reaching awareness. However, sensory overload can occur if the amount of stimuli the brain is receiving is overwhelming to an individual. Sensory deprivation can also occur if there are insufficient sensations from the environment.[26]
Sensory Impairment
Alterations in sensory function include sensory impairment, sensory overload, and sensory deprivation. Sensory impairment includes any type of difficulty that an individual has with one of their five senses. When an individual experiences loss of a sensory function, such as vision, the way they interact with the environment is affected. For example, when an individual gradually loses their vision, their reliance on other senses to receive information from the environment is often enhanced.
Safety is always a nursing consideration for a client with a sensory impairment. Intact senses are required to make decisions about functioning safely within the environment. For example, an individual who has impaired hearing may not be able to hear a smoke alarm and requires visual indicators when the alarm is triggered.
Sensory impairments are very common in older adults. Most older adults develop impaired near vision called presbyopia, resulting in the need for reading glasses. See Figure 7.2[27] for an image of simulated presbyopia.
Deficits in taste and smell are also prevalent in this age group. Additionally, kinesthetic impairment (an altered sense of touch) can occur in adults as young as 55. Kinesthetic impairment can cause difficulty in daily functioning, such as buttoning one’s shirt or performing other fine motor tasks. These sensory losses can greatly impact how older adults live and function.[28]

Vision Impairments
Several types of visual impairments commonly occur in older adults, including macular degeneration, cataracts, glaucoma, diabetic retinopathy, and presbyopia. See Table 7.2 for more information about each of these visual conditions.
Table 7.2 Common Visual Conditions
| Macular Degeneration | Macular degeneration is the leading cause of legal blindness in individuals over 60 years of age. Risk factors include advancing age, a positive family history, hypertension, and smoking. In macular degeneration, there is loss of central vision with classic symptoms such as blurred central vision, distorted vision that causes difficulty driving and reading, and the requirement for brighter lights and magnification for close-up visual activities.[29] |
|---|---|
| Cataracts | Cataracts are the opacity of the lens of the eye that causes clouded, blurred, or dimmed vision. About half of individuals ages 65 to 75 will develop cataracts, with further incidence occurring after age 75. Cataracts can be removed with surgery that replaces the lens with an artificial lens.[30] |
| Glaucoma | Glaucoma is caused by elevated intraocular pressure that leads to progressive damage to the optic nerve, resulting in gradual loss of peripheral vision. It affects about 4% of individuals over age 70.[31] |
| Diabetic Retinopathy | Diabetic retinopathy is the leading cause of blindness in adults diagnosed with type 1 and type 2 diabetes mellitus. Diabetic retinopathy is a complication of diabetes mellitus due to damaged blood vessels in the retina causing vision loss.[32] Clients with diabetes are encouraged to receive annual eye exams so that retinopathy can be discovered and treated early. Treatments, such as laser treatment that can help shrink blood vessels, injections that can reduce swelling, or surgery, can prevent permanent vision loss.[33] |
| Presbyopia | As a person ages, the lens of the eye gradually becomes thicker and loses flexibility. It stops focusing light on the retina correctly, causing impaired near vision and accommodation at all distances. Presbyopia starts in the early to mid-forties and worsens with aging. It can lead to significant visual impairment but does not usually cause blindness.[34] |
Hearing Loss and Ear Problems
Approximately one third of individuals aged 70 and older have hearing loss. Good hearing depends on a series of events that change sound waves in the air into electrical signals. The auditory nerve conducts these electrical signals from the ear to the brain through a series of steps. The structures of the ear, such as the tympanic membrane and cochlea, must be intact and functioning appropriately for conduction of sound to occur. Age-related hearing loss (presbycusis) gradually occurs in most individuals as they age.[35] Typically, low-pitched sounds are easiest to hear, but it often becomes increasingly difficult to hear normal conversation, especially over loud background noise. Hearing aids are commonly used to enhance hearing. See Figure 7.3[36] for an image of common hearing aids used to treat hearing loss.
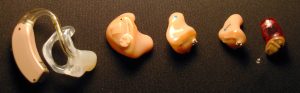
Hearing loss can be caused by other factors in addition to aging. A build-up of ear wax in the ear canal can cause temporary hearing loss. Sounds that are too loud or long-term exposure to loud noises can cause noise-induced hearing loss. For example, a loud explosion or employment using loud machinery without ear protection can damage the sensory hair cells in the ear. After these hair cells are damaged, the ability to hear is permanently diminished. Tinnitus, a medical term for ringing in the ears, can also occur. Some medications, such as high doses of aspirin or loop diuretics, can cause toxic effects to the sensory cells in the ear and lead to hearing loss or tinnitus.[37],[38] In addition to hearing loss, ear problems can also cause problems with balance, dizziness, and vertigo due to vestibular dysfunction.
Kinesthetic Impairments
Kinesthetic impairments, such as peripheral neuropathy, affect the ability to feel sensations. Symptoms of peripheral neuropathy include sensations of pain, burning, tingling, and numbness in the extremities that decrease a person’s ability to feel touch, pressure, and vibration. Position sense can also be affected and makes it difficult to coordinate complex movements, such as walking, fastening buttons, or maintaining balance when one’s eyes are closed. Peripheral neuropathy is caused by nerve damage that commonly occurs in clients with diabetes mellitus or peripheral vascular disease. It can also be caused by physical injuries, infections, autoimmune diseases, vitamin deficiencies, kidney diseases, liver diseases, and certain medications like chemotherapy medications.[39]
Life Span Considerations
Impaired sensory functioning increases the risk for social isolation in older adults. For example, when individuals are not able to hear well, they may pretend to hear in an attempt to avoid embarrassment when asking for the information to be repeated. They may begin to avoid noisy environments or stop participating socially in conversations around them.
Infants and children are also at risk for vision and hearing impairments related to genetic or prenatal conditions. Early determination of sensory impairments is crucial so that problems can be addressed with accommodations to minimize the impact on a child’s development. For example, a screening hearing test is completed on all newborns before discharge to evaluate for hearing impairments that can affect their speech development.
Sensory Overload and Sensory Deprivation
Stimuli are continually received from a variety of sources in our environment and from within our bodies. When an individual receives too many stimuli or cannot selectively filter out meaningful stimuli, sensory overload can occur. Symptoms of sensory overload include irritability, restlessness, covering ears or eyes to shield them from sensory input, and increased sensitivity to tactile input (i.e., scratchy fabric or sensations of medical equipment).[40] Sensory overload affects an individual’s ability to interpret stimuli from their environment and can lead to confusion and agitation. See Figure 7.4[41] of an image of a client reacting to sensory overload.
The health care environment with its frequent noisy alarms, treatments, staff interruptions, and noisy hallway conversations can cause sensory overload for clients. Additionally, the amount of information provided to a client experiencing a health crisis can contribute to sensory overload, such as teaching about procedural and diagnostic testing. Clients may only be able to process small chunks of information provided at a time and may need this information repeated to ensure they understand their situation and retain the information.
Individuals have different tolerances for the amount of stimuli that will affect them adversely. Tolerance to stimuli is impacted by factors such as pain, stress levels, sleep patterns, physical health, and emotional health. When sensory overload occurs in a hospitalized client, it can lead to delirium and acute confusion. It is important for the nurse to limit unnecessary awakenings and interactions with the health care team members when a client is experiencing sensory overload.

Conversely, symptoms of sensory deprivation may occur when there is a lack of sensations due to sensory impairments or few quality stimuli in the client environment. This may include hearing or vision impairments, brain or spinal injuries resulting in lack of tactile sensations, having few or no visitors, or having transmission-based precautions resulting in decreased staff interaction. Interventions such as opening window curtains, providing a clock and calendar for orientation to the time and the day of the week, encouraging visitors, and spending additional time with the client can help prevent sensory deprivation.
Clients with sensory deprivation may experience excessive tiredness or lethargy, disorientation, depression or apathy. People experiencing sensory deprivation often report perceptual disturbances such as hallucinations. Symptoms of sensory deprivation can mimic delirium, so it is important for a nurse to further investigate new perceptual disturbances.[42]
Review information on delirium in Chapter 6.2.
Intravascular fluid loss. Used interchangeably with “deficient fluid volume” and “dehydration.”

